What the study found Most people diagnosed with cancer have pre-existing chronic conditions (also known as comorbidities), which might delay the diagnosis of cancer. To better understand which patient groups […]
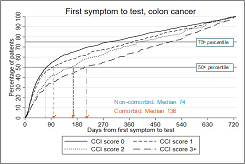

What the study found Most people diagnosed with cancer have pre-existing chronic conditions (also known as comorbidities), which might delay the diagnosis of cancer. To better understand which patient groups […]
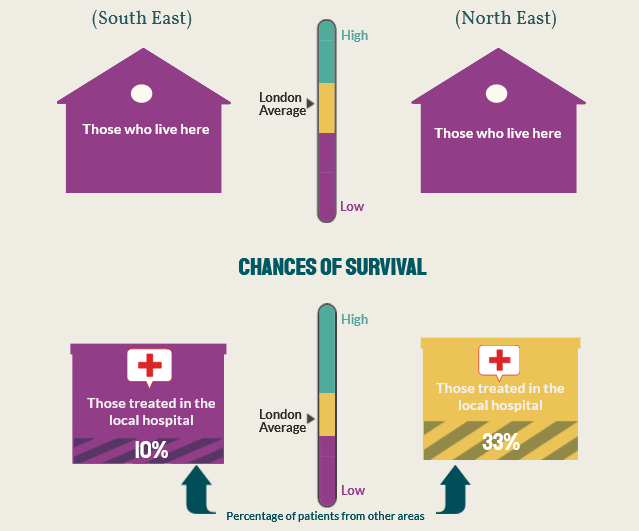
This study highlights the need to better coordinate primary and secondary care sectors in some areas of London to improve timely access to specialised clinicians and diagnostic tests.

In this seminar, Michelle Kelly-Irving will outline the embodiment dynamic conceptual framework used to examine how health inequalities are partly constructed through social-to-biological processes. She will provide empirical examples of […]

Corsican Summer School on Modern Methods in Biostatistics and Epidemiology
4th-8th July 2022
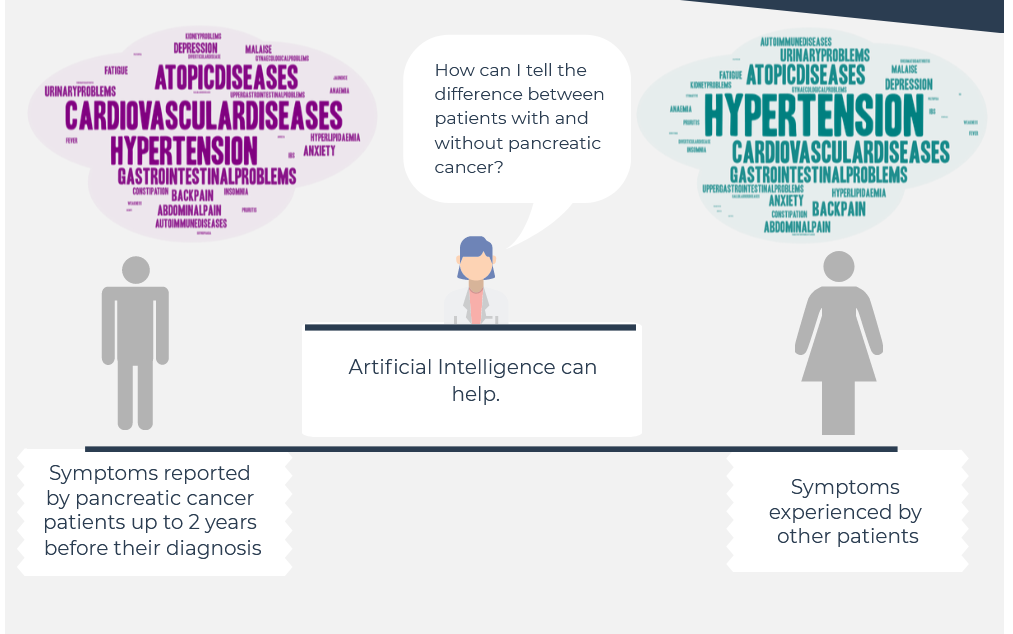
PANCREATIC CANCER PATIENTS are usually diagnosed too LATE for curative treatment because there are no early stage symptoms associated with tumour development.
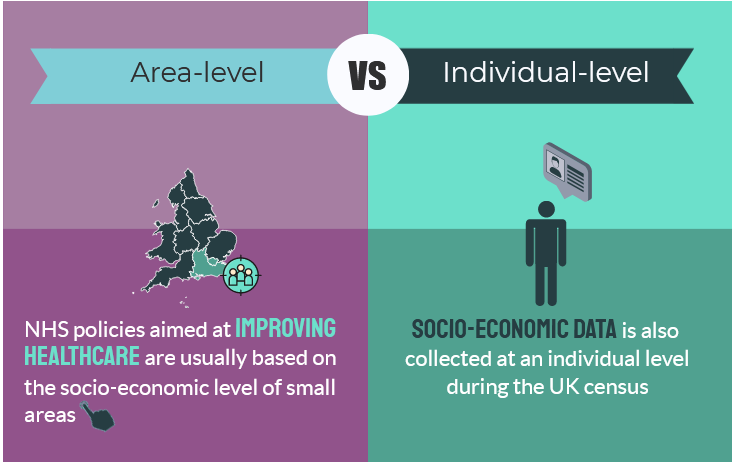
Assessment of the concordance between individual-level and area-level measures of socio-economic deprivation in a cancer patient cohort in England and Wales

Since a national lockdown was introduced across the UK in March, 2020, in response to the COVID-19
pandemic, cancer screening has been suspended, routine diagnostic work deferred, and only urgent symptomatic
cases prioritised for diagnostic intervention.
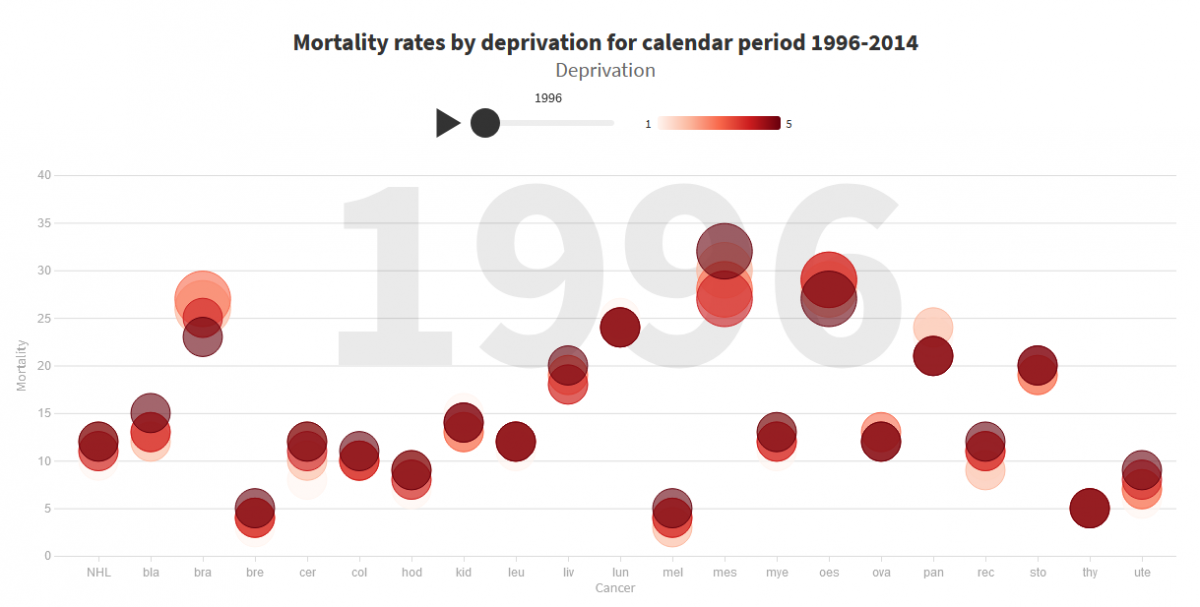
In 1996 a government report showed that there was a difference in how long cancer patients were surviving depending on how wealthy they were (we call it the ‘deprivation gap in survival’).